Advances in understanding cold-related hemodynamic changes in the cardiovascular system
doi: 10.1515/fzm-2026-0005
-
Abstract: Cold exposure induces significant hemodynamic disturbances that contribute to increased morbidity and mortality from cardiovascular disease (CVD). This review explores the physiological and molecular mechanisms by which cold stress affects blood pressure regulation, vascular resistance, and wall shear stress (WSS), and how these alterations promote CVD development. Cold exposure elevates blood pressure primarily through activation of the sympathetic nervous system (SNS) and the renin-angiotensin-aldosterone system (RAAS). These neurohumoral pathways enhance vasoconstriction and increase blood viscosity, thereby elevating peripheral vascular resistance. Moreover, cold-induced alterations in WSS impair endothelial function, facilitate platelet aggregation, and accelerate atherosclerotic progression. Despite extensive evidence linking cold exposure to hemodynamic and vascular dysfunction, the precise molecular and integrative mechanisms remain incompletely understood. We propose that the SNS-RAAS axis represents a central regulatory pathway underlying cold-induced hemodynamic changes, warranting further investigation to clarify its contribution to cold-related cardiovascular pathology.
-
Key words:
- cold /
- hemodynamics /
- blood pressure /
- blood resistance /
- blood shear stress
-
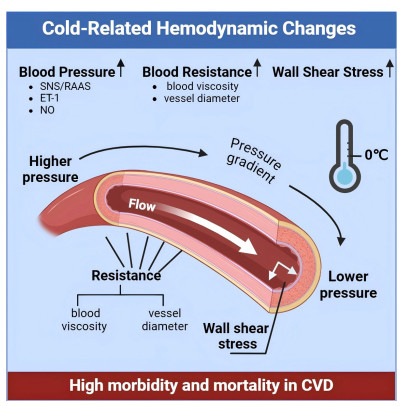
Figure 1. Schematic representation of the effects of cold exposure on hemodynamic factors Created in BioRender.com
Cold exposure activates the sympathetic nervous system (SNS) and reninangiotensin-aldosterone system (RAAS), leading to vasoconstriction, increased blood viscosity, and elevated blood pressure. These changes collectively alter vascular resistance and wall shear stress (WSS), resulting in endothelial dysfunction, enhanced platelet aggregation, and acceleration of atherosclerosis. The SNS/RAAS axis serves as the central regulator linking cold exposure to hemodynamic and cardiovascular disturbances. CVD, cardiovascular diseases; SNS/RAAS, sympathetic nervous system and renin-angiotensin-aldosterone system; ET, Endothelin.
-
[1] Chen R, Yin P, Wang L, et al. Association between ambient temperature and mortality risk and burden: time series study in 272 main Chinese cities. BMJ, 2018; 363: k4306. doi: 10.1136/bmj.k4306 [2] Burkart K G, Brauer M, Aravkin A Y, et al. Estimating the cause-specific relative risks of non-optimal temperature on daily mortality: a two-part modelling approach applied to the Global Burden of Disease Study. Lancet, 2021; 398(10301): 685-697. doi: 10.1016/S0140-6736(21)01700-1 [3] Fu S H, Gasparrini A, Rodriguez P S, et al. Mortality attributable to hot and cold ambient temperatures in India: a nationally representative case-crossover study. PLoS Med, 2018; 15(7): e1002619. doi: 10.1371/journal.pmed.1002619 [4] Macintyre H L, Heaviside C, Cai X, et al. The winter urban heat island: Impacts on cold-related mortality in a highly urbanized European region for present and future climate. Environ Int, 2021; 154: 106530. doi: 10.1016/j.envint.2021.106530 [5] Cheng J, Ho H C, Su H, et al. Low ambient temperature shortened life expectancy in Hong Kong: A time-series analysis of 1.4 million years of life lost from cardiorespiratory diseases. Environ Res, 2021; 201: 111652. doi: 10.1016/j.envres.2021.111652 [6] Gao J, Yu F, Xu Z, et al. The association between cold spells and admissions of ischemic stroke in Hefei, China: modified by gender and age. Sci Total Environ, 2019; 669: 140-147. doi: 10.1016/j.scitotenv.2019.02.452 [7] Qi X, Wang Z, Xia X, et al. The effects of heatwaves and cold spells on patients admitted with acute ischemic stroke. Ann Transl Med, 2021; 9(4): 309. doi: 10.21037/atm-20-4256 [8] Han J, Liu S, Zhang J, et al. The impact of temperature extremes on mortality: a time-series study in Jinan, China. BMJ Open, 2017; 7(4): e014741. doi: 10.1136/bmjopen-2016-014741 [9] Su Y Y, Li H M, Yan Z X, et al. Renin-angiotensin system activation and imbalance of matrix metalloproteinase-9/tissue inhibitor of matrix metalloproteinase-1 in cold-induced stroke. Life Sci, 2019; 231: 116563. doi: 10.1016/j.lfs.2019.116563 [10] Crosswhite P, Sun Z. Ribonucleic acid interference knockdown of interleukin 6 attenuates cold-induced hypertension. Hypertension, 2010; 55(6): 1484-1491. doi: 10.1161/HYPERTENSIONAHA.109.146902 [11] Hollenberg S M. Hemodynamic monitoring. Chest, 2013; 143(5): 1480-1488. doi: 10.1378/chest.12-1901 [12] Fan P, Xue X, Hu J, et al. Ambient temperature and ambulatory blood pressure: An hourly-level, longitudinal panel study. Sci Total Environ, 2023; 864: 160854. doi: 10.1016/j.scitotenv.2022.160854 [13] Umishio W, Ikaga T, Kario K, et al. Cross-sectional analysis of the relationship between home blood pressure and indoor temperature in winter: a nationwide smart wellness housing survey in Japan. Hypertension, 2019; 74(4): 756-766. doi: 10.1161/HYPERTENSIONAHA.119.12914 [14] Huang C C, Chen Y H, Hung C S, et al. Assessment of the relationship between ambient temperature and home blood pressure in patients from a web-based synchronous telehealth care program: a retrospective study. J Med Internet Res, 2019; 21(3): e12369. doi: 10.2196/12369 [15] Hiramatsu K, Yamada T, Katakura M. Acute effects of cold on blood pressure, renin-angiotensin-aldosterone system, catecholamines and adrenal steroids in man [J]. Clin Exp Pharmacol Physiol, 1984; 11(2): 171-179. doi: 10.1111/j.1440-1681.1984.tb00254.x [16] Jansky L, Sramek P, Savlikova J, et al. Change in sympathetic activity, cardiovascular functions and plasma hormone concentrations due to cold water immersion in men. Eur J Appl Physiol Occup Physiol; 1996; 74(1/2): 148-152. doi: 10.1007/BF00376507 [17] Zhang X, Zhang S, Wang C, et al. Effects of moderate strength cold air exposure on blood pressure and biochemical indicators among cardiovascular and cerebrovascular patients. Int J Environ Res Public Health, 2014; 11(3): 2472-2487. doi: 10.3390/ijerph110302472 [18] Marino F, Sockler J M, Fry J M. Thermoregulatory, metabolic and sympathoadrenal responses to repeated brief exposure to cold. Scand J Clin Lab Invest, 1998; 58(7): 537-545. doi: 10.1080/00365519850186157 [19] Cummings M F, Steele P M, Mahar L J, et al. The role of adrenal medullary catecholamine release in the response to a cold pressor test. Cardiovasc Res, 1983; 17(4): 189-191. doi: 10.1093/cvr/17.4.189 [20] Lenders J W, Peters J H, Pieters G F, et al. Hemodynamic reactivity to sympathoadrenal stimulation in adrenalectomized women. J Clin Endocrinol Metab, 1988; 67(1): 139-143. doi: 10.1210/jcem-67-1-139 [21] Celi F S, Brychta R J, Linderman J D, et al. Minimal changes in environmental temperature result in a significant increase in energy expenditure and changes in the hormonal homeostasis in healthy adults. Eur J Endocrinol, 2010; 163(6): 863-872. doi: 10.1530/EJE-10-0627 [22] Fagius J, Kay R. Low ambient temperature increases baroreflexgoverned sympathetic outflow to muscle vessels in humans. Acta Physiol Scand, 1991; 142(2): 201-209. doi: 10.1111/j.1748-1716.1991.tb09148.x [23] Hintsala H E, Kiviniemi A M, Tulppo M P, et al. Hypertension does not alter the increase in cardiac baroreflex sensitivity caused by moderate cold exposure. Front Physiol, 2016; 7: 204. doi: 10.3389/fphys.2016.00204 [24] Yamazaki F, Sone R. Modulation of arterial baroreflex control of heart rate by skin cooling and heating in humans. J Appl Physiol (1985), 2000; 88(2): 393-400. doi: 10.1152/jappl.2000.88.2.393 [25] Sun Z, Cade R, Zhang Z, et al. Angiotensinogen gene knockout delays and attenuates cold-induced hypertension. Hypertension, 2003; 41(2): 322-327. doi: 10.1161/01.HYP.0000050964.96018.FA [26] Peng J F, Kimura B, Fregly M J, et al. Reduction of cold-induced hypertension by antisense oligodeoxynucleotides to angiotensinogen mRNA and AT1- receptor mRNA in brain and blood. Hypertension, 1998; 31(6): 1317-1323. doi: 10.1161/01.HYP.31.6.1317 [27] Wang X, Sun Z, Cade R. Prolonged attenuation of cold-induced hypertension by adenoviral delivery of renin antisense. Kidney Int, 2005; 68(2): 680-687. doi: 10.1111/j.1523-1755.2005.00446.x [28] Sun Z, Wang X, Wood C E, et al. Genetic AT1A receptor deficiency attenuates cold-induced hypertension. Am J Physiol Regul Integr Comp Physiol, 2005; 288(2): R433-R439. doi: 10.1152/ajpregu.00466.2004 [29] Wang X, Cade R, Sun Z. Human eNOS gene delivery attenuates cold-induced elevation of blood pressure in rats. Am J Physiol Heart Circ Physiol, 2005; 289(3): H1161-H1168. doi: 10.1152/ajpheart.01306.2004 [30] Chen G F, Sun Z. Effects of chronic cold exposure on the endothelin system. J Appl Physiol (1985), 2006; 100(5): 1719-1726. doi: 10.1152/japplphysiol.01407.2005 [31] Cai J, Meng X, Wang C, et al. The cold effects on circulatory inflammation, thrombosis and vasoconstriction in type 2 diabetic patients. Sci Total Environ, 2016; 568: 271-277. doi: 10.1016/j.scitotenv.2016.06.030 [32] Sun Z. Cardiovascular responses to cold exposure. Front Biosci (Elite Ed), 2010; 2(2): 495-503. doi: 10.2741/e108 [33] Sun Z, Fregly M J, Cade J R. Effect of renal denervation on elevation of blood pressure in cold-exposed rats. Can J Physiol Pharmacol, 1995; 73(1): 72-78. doi: 10.1139/y95-010 [34] Shechtman O, Fregly M J, Van Bergen P, et al. Prevention of cold-induced increase in blood pressure of rats by captopril. Hypertension, 1991; 17(6 Pt 1): 763-770. doi: 10.1161/01.HYP.17.6.763 [35] Fregly M J, Rossi F, Van Bergen P, et al. Effect of chronic treatment with losartan potassium (DuP 753) on the elevation of blood pressure during chronic exposure of rats to cold. Pharmacology, 1993; 46(4): 198-205. doi: 10.1159/000139046 [36] Jayalalitha G, Shanthoshini D V, Uthayakumar R. Fractal model for blood flow in cardiovascular system. Comput Biol Med, 2008; 38(6): 684-693. doi: 10.1016/j.compbiomed.2008.03.002 [37] Blumberg M S, Sokoloff G, Kent K J. Cardiovascular concomitants of ultRAASound production during cold exposure in infant rats. Behav Neurosci, 1999; 113(6): 1274-1282. doi: 10.1037//0735-7044.113.6.1274 [38] Luo B, Zhang S, Ma S, et al. Effects of cold air on cardiovascular disease risk factors in rat. Int J Environ Res Public Health, 2012; 9(7): 2312-2325. doi: 10.3390/ijerph9072312 [39] Luo B, Zhang S, Ma S, et al. Effects of different cold-air exposure intensities on the risk of cardiovascular disease in healthy and hypertensive rats. Int J Biometeorol, 2014; 58(2): 185-194. doi: 10.1007/s00484-013-0641-3 [40] Keatinge W R, Coleshaw S R, Cotter F, et al. Increases in platelet and red cell counts, blood viscosity, and arterial pressure during mild surface cooling. Factors in mortality from coronary and cerebral thrombosis in winter. Br Med J (Clin Res Ed), 1984; 289(6456): 1405-1408. doi: 10.1136/bmj.289.6456.1405 [41] Frohlich M, Sund M, Russ S, et al. Seasonal variations of rheological and hemostatic parameters and acute-phase reactants in young, healthy subjects. Arterioscler Thromb Vasc Biol, 1997; 17(11): 2692-2697. doi: 10.1161/01.ATV.17.11.2692 [42] Ni W, Schneider A, Wolf K, et al. Short-term effects of cold spells on plasma viscosity: results from the KORA cohort study in Augsburg, Germany. Environ Pollut, 2022; 302: 119071. doi: 10.1016/j.envpol.2022.119071 [43] Kesmarky G, Kenyeres P, Rabai M, et al. Plasma viscosity: a forgotten variable. Clin Hemorheol Microcirc, 2008; 39(1/4): 243-246. doi: 10.3233/CH-2008-1088 [44] Vogelaere P, Pereira C. Thermoregulation and aging. Rev Port Cardiol, 2005; 24(5): 747-761. [45] Young A J, Muza S R, Sawka M N, et al. Human vascular fluid responses to cold stress are not altered by cold acclimation. Undersea Biomed Res, 1987, 14(3): 215-228. [46] Jensen T, Halvorsen S, Godal H C, et al. The viscosity of fibrinogen subfractions and of EDTA denatured fibrinogen do not differ from that of native fibrinogen. Thromb Res, 2004; 113(1): 51-56. doi: 10.1016/j.thromres.2004.01.010 [47] Letcher R L, Chien S, Pickering T G, et al. Direct relationship between blood pressure and blood viscosity in normal and hypertensive subjects. role of fibrinogen and concentration. Am J Med, 1981; 70(6): 1195-1202. doi: 10.1016/0002-9343(81)90827-5 [48] Matsuda T, Murakami M. Relationship between fibrinogen and blood viscosity. Thromb Res, 1976; 8(2 Suppl): 25-33. doi: 10.1016/0049-3848(76)90044-X [49] Van Der Bom J G, De Maat M P, Bots M L, et al. Seasonal variation in fibrinogen in the Rotterdam Study. Thromb Haemost, 1997; 78(3): 1059-1062. doi: 10.1055/s-0038-1657687 [50] Woodhouse P R, Khaw K T, Plummer M, et al. Seasonal variations of plasma fibrinogen and factor Ⅶ activity in the elderly: winter infections and death from cardiovascular disease. Lancet, 1994; 343(8895): 435-439. doi: 10.1016/S0140-6736(94)92689-1 [51] Neild P J, Syndercombe-Court D, Keatinge W R, et al. Cold-induced increases in erythrocyte count, plasma cholesterol and plasma fibrinogen of elderly people without a comparable rise in protein C or factor X. Clin Sci (Lond), 1994; 86(1): 43-48. doi: 10.1042/cs0860043 [52] Nagelkirk P R, Hogan K B, Hoare J M. Ambient temperature affects thrombotic potential at rest and following exercise. Thromb Res, 2012; 130(2): 248-252. doi: 10.1016/j.thromres.2011.10.015 [53] Holmes G L, Thompson J L. Effects of kainic acid on seizure susceptibility in the developing brain. Brain Res, 1988; 467(1): 51-59. doi: 10.1016/0165-3806(88)90066-1 [54] Alba B K, Castellani J W, Charkoudian N. Cold-induced cutaneous vasoconstriction in humans: function, dysfunction and the distinctly counterproductive. Exp Physiol, 2019; 104(8): 1202-1214. doi: 10.1113/EP087718 [55] Zhang D, Chang S, Jing B, et al. Reactive oxygen species are essential for vasoconstriction upon cold exposure. Oxid Med Cell Longev, 2021; 2021: 8578452. doi: 10.1155/2021/8578452 [56] Wigley F M, Flavahan N A. Raynaud's Phenomenon. N Engl J Med, 2016; 375(6): 556-565. doi: 10.1056/NEJMra1507638 [57] Stephens D P, Aoki K, Kosiba W A, et al. Nonnoradrenergic mechanism of reflex cutaneous vasoconstriction in men. Am J Physiol Heart Circ Physiol, 2001; 280(4): H1496-H1504. doi: 10.1152/ajpheart.2001.280.4.H1496 [58] Taher M, Gholampour S. Effect of ambient temperature changes on blood flow in anterior cerebral artery of patients with skull prosthesis. World Neurosurg, 2020; 135: e358-e365. doi: 10.1016/j.wneu.2019.11.171 [59] Binti Md Isa K, Kawasaki N, Ueyama K, et al. Effects of cold exposure and shear stress on endothelial nitric oxide synthase activation. Biochem Biophys Res Commun, 2011; 412(2): 318-322. doi: 10.1016/j.bbrc.2011.07.092 [60] Zhang J N, Wood J, Bergeron A L, et al. Effects of low temperature on shear-induced platelet aggregation and activation. J Trauma, 2004, 57(2): 216-223. [61] Gnasso A, Carallo C, Irace C, et al. Association between wall shear stress and flow-mediated vasodilation in healthy men. Atherosclerosis, 2001; 156(1): 171-176. doi: 10.1016/S0021-9150(00)00617-1 [62] Yang L, Li L, Lewington S, et al. Outdoor temperature, blood pressure, and cardiovascular disease mortality among 23 000 individuals with diagnosed cardiovascular diseases from China. Eur Heart J, 2015; 36(19): 1178-1185. doi: 10.1093/eurheartj/ehv023 [63] Hanazawa T, Asayama K, Watabe D, et al. Association between amplitude of seasonal variation in self-measured home blood pressure and cardiovascular outcomes: the HOMED-BP (Hypertension Objective Treatment Based on Measurement By Electrical Devices of Blood Pressure) study. J Am Heart Assoc, 2018; 7(10): e008509. doi: 10.1161/JAHA.117.008509 [64] Peters S A, Woodward M, Rumley A, et al. Plasma and blood viscosity in the prediction of cardiovascular disease and mortality in the Scottish Heart Health Extended Cohort Study. Eur J Prev Cardiol, 2017; 24(2): 161-167. doi: 10.1177/2047487316672004 [65] Zhou M, Yu Y, Chen R, et al. Wall shear stress and its role in atherosclerosis. Front Cardiovasc Med, 2023; 10: 1083547. doi: 10.3389/fcvm.2023.1083547 -


 投稿系统
投稿系统


 下载:
下载: