Cold exposure aggravates myocardial ischemia-reperfusion injury via m6A-mediated circRNA-mRNA regulatory networks
doi: 10.1515/fzm-2026-0001
-
Abstract:
Objective Myocardial ischemia-reperfusion (I/R) injury remains a major contributor to cardiac morbidity and mortality, and accumulating evidence suggests that epitranscriptomic regulation may critically influence cardiac stress responses. N6-methyladenosine (m6A) modification and circular RNAs (circRNAs) have emerged as important regulators of cardiovascular pathology; however, their integrated roles in myocardial I/R injury, particularly under chronic cold stress, remain poorly defined. Methods A mouse model of myocardial I/R injury was established under room-temperature or chronic cold exposure conditions. Cardiac function, infarct size, histopathology, and serum injury markers were assessed. Global m6A levels were quantified, and m6A-modified circRNA profiles were analyzed using epitranscriptomic microarrays and bioinformatics approaches. Differentially expressed circRNAs were validated in vivo and in hypoxia-reoxygenation-treated neonatal cardiomyocytes. Circular structures and stability were confirmed by Sanger sequencing, divergent/convergent PCR, and actinomycin D assays. Competing endogenous RNA (ceRNA) networks were constructed to identify downstream regulatory pathways. Results Myocardial I/R injury resulted in significant cardiac dysfunction, increased infarct size, histological damage, and elevated serum CK-MB and LDH levels, accompanied by a marked increase in global m6A methylation. Epitranscriptomic profiling identified 391 circRNAs with altered m6A modification following I/R injury, involving pathways related to molecular binding, cellular processes, and kinase signaling. Multiple circRNAs exhibited consistent dysregulation in both in vivo and in vitro I/R models and displayed high structural stability. Importantly, chronic cold exposure significantly exacerbated I/R-induced cardiac dysfunction and infarct severity while further modulating the expression of specific m6A-modified circRNAs. ceRNA network analysis revealed that cold-responsive circRNAs potentially regulate myocardial injury through miRNA-mediated signaling pathways. Conclusion This study identifies m6A-modified circRNAs as key epitranscriptomic regulators of myocardial I/R injury and demonstrates that chronic cold stress amplifies circRNA-mediated regulatory networks. These findings provide novel mechanistic insight into temperature-dependent epigenetic regulation in ischemic heart disease and highlight m6A-circRNAs as potential therapeutic targets. -
Key words:
- circRNAs /
- m6A /
- myocardial I/R injury /
- cold stress
-
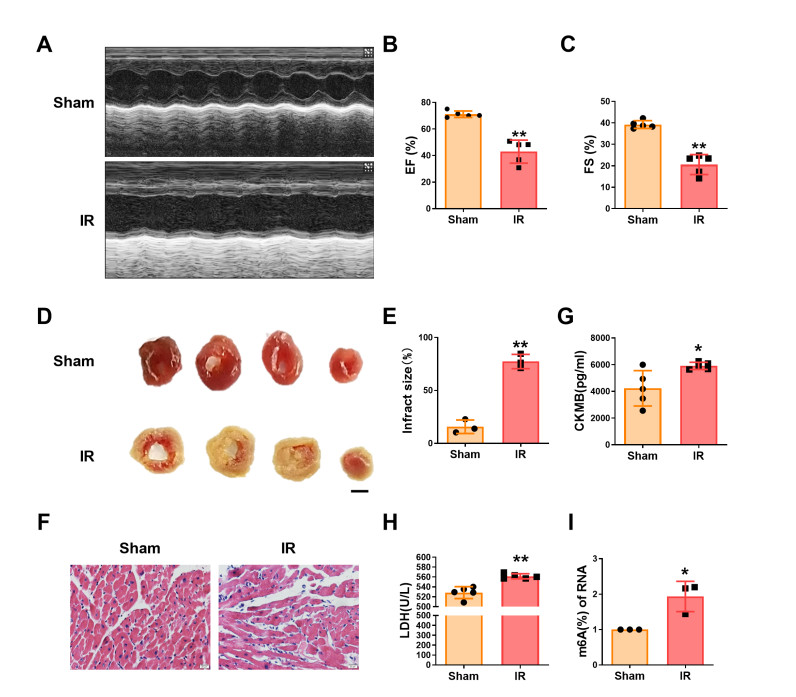
Figure 1. Establishment of a mouse myocardial ischemia-reperfusion (I/R) model
(A) Representative echocardiographic images showing cardiac function. Ejection fraction (EF%). (C) Fractional shortening (FS%). **P < 0.01 versus Sham, N = 5. (D-E) Representative images and quantitative analysis of infarct size assessed by blue-2, 3, 5-triphenyl tetrazolium chloride (TTC) staining. **P < 0.01 versus Sham, N = 3. (F) Representative H&E-stained sections showing myocardial histopathological changes. (G-H) Serum levels of creatine kinase-MB (CK-MB) and lactate dehydrogenase (LDH). *P < 0.05, **P < 0.01 versus Sham, N = 5. (I) Global N6-methyladenosine (m6A) modification levels in cardiac tissue, *P < 0.05 versus Sham, N = 3.
Figure 2. Differential N6-methyladenosine (m6A)-methylated circRNAs and Gene Ontology (GO) pathway analysis
(A) m6A-circRNA epitranscriptomic microarray and bioinformatics analysis showing differential m6A modification levels. N = 3. (B) Scatter plot analysis of differentially expressed circRNAs. (C) Volcano plot analysis of differentially expressed circRNAs. (D) Venn diagram showing circRNAs targeting common miRNAs. (E, F) Distribution of hypermethylated and hypomethylated circRNAs in myocardial I/R injury.
Figure 3. Gene Ontology and pathway enrichment analysis of differentially expressed circRNAs in biological processes, cellular components, and molecular functions
(A-C) Gene Ontology (GO) enrichment analysis of differentially expressed circRNAs in biological processes, cellular components, and molecular functions.(D) Kyoto Encyclopedia of Genes and Genomes (KEGG) pathway enrichment analysis of differentially expressed genes.
Figure 5. Validation of the circular structure of circRNAs
(A, D) Identification of circRNA back-splice junctions by Sanger sequencing. (B, E) Validation of circular structures using divergent and convergent primers with cDNA and genomic DNA templates. (C, F) CircRNA stability assessed by actinomycin D treatment. N = 3-4.
Figure 6. Dynamic changes in N6-methyladenosine (m6A)-circRNA expression in chronic cold stress-induced I/R mice
(A) Baseline echocardiographic assessment of cardiac function. (B) Ejection fraction (EF%). (C) FS%. N = 8. (D) Echocardiographic assessment after four weeks of cold exposure. (E) EF%. (F) FS%. *P < 0.05, **P < 0.01 versus Sham, N = 5. (G-I) Representative images and quantitative analysis of myocardial injury assessed by Evans blue-TTC double staining. *P < 0.05 versus RT-I/R, N = 4.
Figure 7. Expression of N6-methyladenosine (m6A)-methylated circRNAs in chronic cold stress-induced myocardial I/R injury
(A) Relative expression levels of circRNAs in cardiac tissue. *P < 0.05, **P < 0.01 versus RT-Sham, #P < 0.05, ##P < 0.01 versus Cold-Sham, & P < 0.05, & & P < 0.01 versus Cold-I/R N = 4.
Figure 8. Downstream target analysis of cold-responsive circRNAs
(A) Kyoto Encyclopedia of Genes and Genomes (KEGG) pathway enrichment analysis of cold-responsive circRNAs. (B) ceRNA network of five cold-responsive circRNAs and their sponge miRNAs under cold stress conditions. CircRNAs are shown as orange nodes, miRNAs as green nodes, and downstream target genes as blue nodes.
-
[1] Liu C, Li Z, Li B, et al. Relationship between ferroptosis and mitophagy in cardiac ischemia reperfusion injury: A mini-review. Peer J, 2023; 11: e14952. doi: 10.7717/peerj.14952 [2] Ye J, Wang R, Wang M, et al. Hydroxysafflor yellow A ameliorates myocardial ischemia/reperfusion injury by suppressing calcium overload and apoptosis. Oxid Med Cell Longev, 2021; 2021: 6643615. doi: 10.1155/2021/6643615 [3] Algoet M, Janssens S, Himmelreich U, et al. Myocardial ischemia-reperfusion injury and the influence of inflammation. Trends Cardiovasc Med, 2023; 33(6): 357-366. doi: 10.1016/j.tcm.2022.02.005 [4] Tian H, Zhao X, Zhang Y, et al. Abnormalities of glucose and lipid metabolism in myocardial ischemia-reperfusion injury. Biomed Pharmacother, 2023; 163: 114827. doi: 10.1016/j.biopha.2023.114827 [5] Oerum S, Meynier V, Catala M, et al. A comprehensive review of m6A/m6Am RNA methyltransferase structures. Nucleic Acids Res, 2021; 49(13): 7239-7255. doi: 10.1093/nar/gkab378 [6] Qin Y, Li L, Luo E, et al. Role of m6A RNA methylation in cardiovascular disease (Review). Int J Mol Med, 2020; 46(6): 1958-1972. doi: 10.3892/ijmm.2020.4746 [7] Zaccara S, Ries R J, Jaffrey S R. Reading, writing and erasing mRNA methylation. Nat Rev Mol Cell Biol, 2019; 20(10): 608-624. doi: 10.1038/s41580-019-0168-5 [8] Chen Y S, Ouyang X P, Yu X H, et al. N6-adenosine methylation (m(6) A) RNA modification: An emerging role in cardiovascular diseases. J Cardiovasc Transl Res, 2021; 14(5): 857-872. doi: 10.1007/s12265-021-10108-w [9] Ju J, Song Y N, Chen X Z, et al. circRNA is a potential target for cardiovascular diseases treatment. Mol Cell Biochem, 2022; 477(2): 417-430. doi: 10.1007/s11010-021-04286-z [10] Misir S, Wu N, Yang B B. Specific expression and functions of circular RNAs. Cell Death Differ, 2022; 29(3): 481-491. doi: 10.1038/s41418-022-00948-7 [11] Huang A, Zheng H, Wu Z, et al. Circular RNA-protein interactions: Functions, mechanisms, and identification. Theranostics, 2020; 10(8): 3503-3517. doi: 10.7150/thno.42174 [12] Shi Y, Jia X, Xu J. The new function of circRNA: Translation. Clin Transl Oncol, 2020; 22(12): 2162-2169. doi: 10.1007/s12094-020-02371-1 [13] Bai M, Pan C L, Jiang G X, et al. CircHIPK3 aggravates myocardial ischemia-reperfusion injury by binding to miRNA-124-3p. Eur Rev Med Pharmacol Sci, 2019; 23(22): 10107-10114. [14] Jin A, Zhang Q, Cheng H, et al. Circ_0050908 up-regulates TRAF3 by sponging miR-324-5p to aggravate myocardial ischemia-reperfusion injury. Int Immunopharmacol, 2022; 108: 108740. doi: 10.1016/j.intimp.2022.108740 [15] Yin Z, Ding G, Chen X, et al. Beclin1 haploinsufficiency rescues low ambient temperature-induced cardiac remodeling and contractile dysfunction through inhibition of ferroptosis and mitochondrial injury. Metabolism, 2020; 113: 154397. doi: 10.1016/j.metabol.2020.154397 [16] Liu C, Yavar Z, Sun Q. Cardiovascular response to thermoregulatory challenges. Am J Physiol Heart Circ Physiol, 2015; 309(11): H1793-1812. doi: 10.1152/ajpheart.00199.2015 [17] Vuori I. The heart and the cold. Ann Clin Res, 1987; 19(3): 156-162. [18] Chen C W, Wu C H, Liou Y S, et al. Roles of cardiovascular autonomic regulation and sleep patterns in high blood pressure induced by mild cold exposure in rats. Hypertens Res, 2021; 44(6): 662-673. doi: 10.1038/s41440-021-00619-z [19] Näyhä S. Cold and the risk of cardiovascular diseases. A review. Int J Circumpolar Health, 2002; 61(4): 373-380. doi: 10.3402/ijch.v61i4.17495 [20] Kusserow A, Pang K, Sturm C, et al. Unexpected complexity of the Wnt gene family in a sea anemone. Nature, 2005; 433(7022): 156-160. doi: 10.1038/nature03158 [21] Zhao Z, Li X, Gao C, et al. Peripheral blood circular RNA hsa_ circ_0124644 can be used as a diagnostic biomarker of coronary artery disease. Sci Rep, 2017; 7: 39918. doi: 10.1038/srep39918 [22] Wu H, Jiang W, Pang P, et al. m(6)A reader YTHDF1 promotes cardiac fibrosis by enhancing AXL translation. Front Med, 2024; 18(3): 499-515. doi: 10.1007/s11684-023-1052-4 [23] Yellon D M, Hausenloy D J. Myocardial reperfusion injury. N Engl J Med, 2007; 357(11): 1121-1135. doi: 10.1056/NEJMra071667 [24] Gong R, Wang X, Li H, et al. Loss of m(6)A methyltransferase METTL3 promotes heart regeneration and repair after myocardial injury. Pharmacol Res, 2021; 174 105845. doi: 10.1016/j.phrs.2021.105845 [25] Wang X, Zhao B S, Roundtree I A, et al. N(6)-methyladenosine modulates messenger RNA translation efficiency. Cell, 2015; 161(6): 1388-1399. doi: 10.1016/j.cell.2015.05.014 [26] Dominissini D, Moshitch-Moshkovitz S, Schwartz S, et al. Topology of the human and mouse m6A RNA methylomes revealed by m6A-seq. Nature, 2012; 485(7397): 201-206. doi: 10.1038/nature11112 [27] Kumari R, Ranjan P, Suleiman Z G, et al. mRNA modifications in cardiovascular biology and disease: With a focus on m6A modification. Cardiovasc Res, 2022; 118(7): 1680-1692. doi: 10.1093/cvr/cvab160 [28] Zhang M, Shi J, Zhou J, et al. N6-methyladenosine methylation mediates non-coding RNAs modification in microplastic-induced cardiac injury. Ecotoxicol Environ Saf, 2023; 262 115174. doi: 10.1016/j.ecoenv.2023.115174 [29] Zhang J, Luo C J, Xiong X Q, et al. MiR-21-5p-expressing bone marrow mesenchymal stem cells alleviate myocardial ischemia/reperfusion injury by regulating the circRNA_0031672/miR-21-5p/programmed cell death protein 4 pathway. J Geriatr Cardiol, 2021; 18(12): 1029-1043. [30] Sanger H L, Klotz G, Riesner D, et al. Viroids are single-stranded covalently closed circular RNA molecules existing as highly base-paired rod-like structures. Proc Natl Acad Sci U S A, 1976; 73(11): 3852-3856. doi: 10.1073/pnas.73.11.3852 [31] Wang L, Feng J, Feng X, et al. Exercise-induced circular RNA circUtrn is required for cardiac physiological hypertrophy and prevents myocardial ischaemia-reperfusion injury. Cardiovasc Res, 2023; 119(16): 2638-2652. doi: 10.1093/cvr/cvad161 [32] Tan J, Min J, Jiang Y, et al. CircCHSY1 protects hearts against ischemia/reperfusion injury by enhancing heme oxygenase 1 expression via miR-24-3p. Cardiovasc Res, 2024; [33] Zhou W Y, Cai Z R, Liu J, et al. Circular RNA: Metabolism, functions and interactions with proteins. Mol Cancer, 2020; 19(1): 172. doi: 10.1186/s12943-020-01286-3 [34] Wang D, Tian L, Wang Y, et al. Circ_0001206 regulates miR-665/CRKL axis to alleviate hypoxia/reoxygenation-induced cardiomyocyte injury in myocardial infarction. ESC Heart Fail, 2022; 9(2): 998-1007. doi: 10.1002/ehf2.13725 [35] Nirwane A, Majumdar A. Understanding mitochondrial biogenesis through energy sensing pathways and its translation in cardio-metabolic health. Arch Physiol Biochem, 2018; 124(3): 194-206. doi: 10.1080/13813455.2017.1391847 [36] Cheng X, Su H. Effects of climatic temperature stress on cardiovascular diseases. Eur J Intern Med, 2010; 21(3): 164-167. doi: 10.1016/j.ejim.2010.03.001 [37] Shor E, Roelfs D. Climate shock: Moving to colder climates and immigrant mortality. Soc Sci Med, 2019; 235 112397. doi: 10.1016/j.socscimed.2019.112397 [38] Mercer J B. Cold—an underrated risk factor for health. Environ Res, 2003; 92(1): 8-13. doi: 10.1016/S0013-9351(02)00009-9 [39] Yu W, Mengersen K, Wang X, et al. Daily average temperature and mortality among the elderly: A meta-analysis and systematic review of epidemiological evidence. Int J Biometeorol, 2012; 56(4): 569-581. doi: 10.1007/s00484-011-0497-3 [40] Alba B K, Castellani J W, Charkoudian N. Cold-induced cutaneous vasoconstriction in humans: Function, dysfunction and the distinctly counterproductive. Exp Physiol, 2019; 104(8): 1202-1214. doi: 10.1113/EP087718 [41] Medina-Ramón M, Zanobetti A, Cavanagh D P, et al. Extreme temperatures and mortality: Assessing effect modification by personal characteristics and specific cause of death in a multi-city case-only analysis. Environ Health Perspect, 2006; 114(9): 1331-1336. doi: 10.1289/ehp.9074 [42] Song X, Wang S, Hu Y, et al. Impact of ambient temperature on morbidity and mortality: An overview of reviews. Sci Total Environ, 2017; 586 241-254. doi: 10.1016/j.scitotenv.2017.01.212 [43] Chen G F, Sun Z. Effects of chronic cold exposure on the endothelin system. J Appl Physiol (1985), 2006; 100(5): 1719-1726. doi: 10.1152/japplphysiol.01407.2005 [44] Yin Y, Zhang F, Feng S, et al. Activation mechanism of the mouse cold-sensing TRPM8 channel by cooling agonist and PIP(2). Science, 2022; 378(6616): eadd1268. doi: 10.1126/science.add1268 [45] Yang S, Ma H, Wang L, et al. The role of β3-adrenergic receptors in cold-induced beige adipocyte production in pigs. Cells, 2024; 13(8): 709. doi: 10.3390/cells13080709 [46] Rahbani J F, Bunk J, Lagarde D, et al. Parallel control of cold-triggered adipocyte thermogenesis by UCP1 and CKB. Cell Metab, 2024; 36(3): 526-540. e527. doi: 10.1016/j.cmet.2024.01.001 [47] Gordon C J. The mouse thermoregulatory system: Its impact on translating biomedical data to humans. Physiol Behav, 2017; 179 55-66. doi: 10.1016/j.physbeh.2017.05.026 [48] Fischer A W, Cannon B, Nedergaard J. Optimal housing temperatures for mice to mimic the thermal environment of humans: An experimental study. Mol Metab, 2018; 7: 161-170. doi: 10.1016/j.molmet.2017.10.009 -


 投稿系统
投稿系统


 下载:
下载: